MEDICARE 101 PART 2: MEDICARE PART A
MEDICARE PART A COVERS FOUR MAIN AREAS:

INPATIENT HOSPITALIZATION
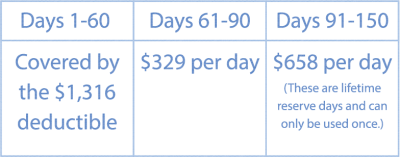
The inpatient hospitalization deductible resets after 60 days of no utilization. This means if there is less than a 60-day break from one hospitalization to another, regardless of the reason for the hospitalization, the initial deductible will cover the subsequent occurrence. If there is a 60+ day break between hospitalizations, the beneficiary will owe the deductible again.
SKILLED NURSING REHABILITATION
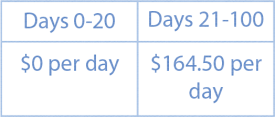
This care is for between an inpatient hospitalization and going to their home.
Same as the inpatient hospitalization deductible, these costs reset after 60 days of no utilization.
There is a three-day hospital stay required to qualify for the skilled nursing benefit.
HOME HEALTHCARE AND HOSPICE
Both are covered 100% by Medicare and both must be doctor ordered to receive benefits.
MEDICARE PART A PREMIUM
Medicare Part A is funded through FICA taxes (through employer payroll for most).
For most, there is no monthly premium for Medicare Part A, provided they have worked 40 quarters (10 years) or can draw off benefits through someone who has (such as a spouse or parent).
Individuals may buy into Medicare Part A if they cannot draw benefits through another. They may call or visit a Social Security office for details.
OTHER MEDICARE PART A INFORMATION
The Medicare Part A inpatient hospitalization deductible may not cover all hospital costs, namely doctor or specialist services which can be billed through Medicare Part B (covered in the next section).
FLASHCARDS! HOVER OVER EACH CARD
TO SEE THE CORRECT ANSWER
What are the 4 main areas covered by Medicare Part A?
Skilled Nursing Rehabilitation
Home Healthcare
Hospice Care
